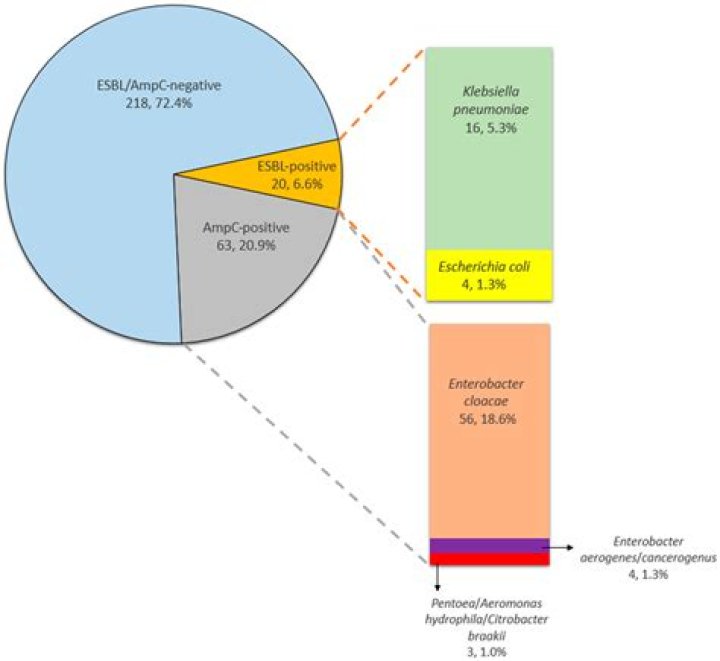
There is no fundamental difference between ESBL and/or AmpC-producing bacteria and other bacteria (e.g. Salmonella). This means that it is possible for the chicks to have acquired the pathogen in the hatchery so that they already carry the bacteria when they are released into the production area.
What is AmpC infection?
WHAT IS AmpC? AmpC is an enzyme which works in a similar way to ESBL but is rarer. If an infection is caused by bacteria producing the AmpC enzyme it may be more difficult to treat. HOW DID I ACQUIRE IT? The bacteria are usually ‘COLONISED’ in patients and are often found in the bowel without causing.
What are AmpC producing bacteria?
Many organisms have inducible AmpC production, most commonly E. cloacae, Klebsiella aerogenes, C. freundii, S. marcescens, Providencia stuartii, P. aeruginosa, Hafnia alvei, and Morganella morganii, often referred to as the ESCPM, SPACE, or SPICE organisms.
Is ESBL the same as cre?
Enterobacteriaceae that are resistant to carbapenems by any mechanism are called carbapenem-resistant Enterobacteriaceae (CRE) (those that produce carbapenemases are called ‘carbapenemase-producing Enterobacteriaceae’ (CPE)) and Enterobacteriaceae that produce ESBL enzymes are called ‘ESBLs’.What is AmpC stand for?
AcronymDefinitionAMPCAssociated Mail & Parcel CentersAMPCAutomatic Mail Processing Centre (India)AMPCAutomatic Message Processing CenterAMPCclass C Betalactamse
How is AmpC treated?
Carbapenems can usually be used to treat infections due to AmpC-producing bacteria, but carbapenem resistance can arise in some organisms by mutations that reduce influx (outer membrane porin loss) or enhance efflux (efflux pump activation).
Is AmpC a gene?
Transmissible plasmids have acquired genes for AmpC enzymes, which consequently can now appear in bacteria lacking or poorly expressing a chromosomal bla(AmpC) gene, such as Escherichia coli, Klebsiella pneumoniae, and Proteus mirabilis.
What does ESBL in urine mean?
ESBL stands for extended spectrum beta-lactamase. It’s an enzyme found in some strains of bacteria. ESBL-producing bacteria can’t be killed by many of the antibiotics that doctors use to treat infections, like penicillins and some cephalosporins. This makes it harder to treat.Is ESBL gram negative?
ESBLs represent an impressive example of the ability of gram-negative bacteria to develop new antibiotic-resistance mechanisms in the face of the introduction of new antimicrobial agents.
How did I get ESBL in my urine?Most ESBL infections are spread by direct contact with an infected person’s bodily fluids (blood, drainage from a wound, urine, bowel movements, or phlegm). They can also be spread by contact with equipment or surfaces that have been contaminated with the germ.
Article first time published onCan you use Cefepime for AmpC?
Conclusions: Cefepime may be a reasonable option for the treatment of invasive infections due to AmpC β-lactamase-producing organisms, particularly when adequate source control is achieved.
Does Klebsiella aerogenes have chromosomal AmpC?
Chromosomally encoded ampC genes can be identified in a number of gram-negative organisms, including E. cloacae, Klebsiella (formerly Enterobacter) aerogenes, C. freundii, S.
Does Proteus mirabilis produce AmpC?
Proteus mirabilis strains that produce extended-spectrum β-lactamase (ESBL), AmpC β-lactamase, and carbapenemase pose potential threats to patient care because most clinical diagnostic laboratories may not attempt to detect these three major groups of enzymes.
What does AMP mean in medical terms?
Amplified musculoskeletal pain syndrome (AMPS) is a very painful medical condition that can cause pain anywhere in the body. These episodes of pain can be intermittent or constant, can affect the whole body or be localized to one area of the body or affect just a limb.
What is AmpC Bible?
The Amplified Bible (AMP) is an English language translation of the Bible produced jointly by Zondervan and The Lockman Foundation. The first edition was published in 1965. It is largely a revision of the American Standard Version of 1901, with reference made to various texts in the original languages.
How is ESBL infection treated?
Infections caused by ESBL-producing germs are treated with antibiotics, but because they are resistant to many commonly prescribed antibiotics, treatment options might be limited. People with these infections sometimes need to be hospitalized for treatment with IV antibiotics.
Does Acinetobacter produce AmpC?
Several other studies have also reported AmpC β-lactamase positive Acinetobacter spp.14,15,16,17. In this study, 84 (61.76%) and 82 (60.29%) isolates were determined as AmpC producers by modified three dimensional and boronic acid inhibitor methods, respectively.
Is AmpC a beta lactamase?
AmpC β-lactamases are clinically important cephalosporinases encoded on the chromosome of many Enterobacteriaceae and a few other organisms where they mediate resistance to cephalothin, cefazolin, cefoxitin, most penicillins, and β-lactamase inhibitor/β-lactam combinations.
How do you measure AmpC production?
- After overnight incubation, examine the plate for either an indentation or a flattening of the zone of inhibition.
- If there is any zone of inhibition, it indicates enzymatic inactivation of cefoxitin (positive result)
Where is Klebsiella aerogenes found?
K. aerogenes is generally found in the human gastrointestinal tract and does not generally cause disease in healthy individuals. It has been found to live in various wastes, hygienic chemicals, and soil.
Does aminoglycosides cover Esbl?
Since aminoglycosides are active against ESBL-EB, and are used as monotherapy in UTI, we conducted a retrospective cohort study to evaluate the efficacy and safety of aminoglycoside monotherapy as definitive treatment in ESBL-EB BSI of urinary origin.
How do you treat C resistant resistance?
AmpC producers are resistant to cephamycins, but cefepime is an option. In the case of carbapenemase-producing Enterobacteriaceae (CPE), only some “second-line” drugs, such as polymyxins, tigecycline, aminoglycosides, and fosfomycin, may be active; double carbapenems can also be considered in specific situations.
Is ESBL gram positive?
Extended spectrum β-lactamases (ESBLs) are enzymes produced by a variety of Gram negative bacteria which confer an increased resistance to commonly used antibiotics.
How do you identify ESBL?
Many tests have been recommended for the detection of ESBL production in vitro. The most commonly used methods include double disc synergy test, combined disc method and E-test. Several automated systems have also been developed for detection and some laboratories use molecular methods for detection of ESBL phenomenon.
How many types of ESBL are there?
ESBLs can be grouped into three main types: TEM, SHV or CTX-M. Another class of β-lactamases, the AmpC β-lactamases, confer resistance to third-generation cephalosporins and cephamycins (eg, cefoxitin).
Can you get rid of ESBL in urine?
If you test positive for ESBL bacterial colonization, you usually will not get treated. This is because no treatment is necessary. Any treatment could cause more antibiotic resistance. In some cases, your body can get rid of the germs on its own.
Is ESBL worse than MRSA?
‘Bacteria of the family enterobacteriaceae, such as Escherichia coli and Klebsiella pneumoniae, which produce extended-spectrum beta-lactimase, are basically no more dangerous than multi-resistant Staphylococcus aureus, with the exception of risk groups such as older patients, where ESBL pathogens can lead to severe …
How does ESBL affect the body?
Bacteria That Produce ESBLs coli strains and types are harmless, but some of them can cause infections leading to stomach pains and diarrhea. Klebsiella pneumoniae may make its way to other parts of your body, causing various infections like pneumonia and urinary tract infections — or UTIs.
Can ESBL cause kidney failure?
ESBLs can cause urinary tract infections (affecting the kidney and bladder), pneumonia (affecting the lungs), wound infections, or life-threatening bloodstream infections. How are ESBL spread?
Is ESBL life long?
ESBL-producing bacteria can live on surfaces for days, weeks and months. It is important to clean surfaces often with a disinfectant.
How serious is ESBL?
ESBL infections are serious and can be life-threatening. Treatment may require hospital stays and long-term follow-up care. The stronger antibiotic medicines used to treat ESBL can cause side effects, such as nausea and diarrhea. The infection can worsen if there is any delay in treatment.